Life’s been pretty good, overall, since I shook the dust of Scarborough off my shoes, and returned to my old Danforth stomping grounds.  It’s such a treat to just walk up the street to a good restaurant, or to pop into a local bar to hear friends playing. I no longer have to pack my purse with overnight supplies before heading out to do groceries, or to visit my chums in the downtown core.
It’s such a treat to just walk up the street to a good restaurant, or to pop into a local bar to hear friends playing. I no longer have to pack my purse with overnight supplies before heading out to do groceries, or to visit my chums in the downtown core.
This retirement stuff seems to be working out just fine! I am totally down for the ‘Live, Love, Laugh” groove.
One aspect to the whole getting older/taking better care of one’s fragile corporeal self has been a downer … who knew all these bits and pieces needed maintenance or they would wear out? Sit down, keener nerdling, yeah, you knew, but I had more fun on the ride.
Bodies wear out, minds get warped, it’s all in the game. Some cope better than others; some win the genetic lottery. The rest seek relief at the hands of professionals, and even some gifted amateurs.
Shelley Marshall is a talented, award winning, comedienne, actress, keynote speaker and producer. She’s also the doyenne of The Mental Wellness Living Loft,  a comfy place for those who’ve been bruised by life to relax, meet other people of like minds, or to simply sit quietly, knitting or colouring, without fear of being asked to ‘move along.’
a comfy place for those who’ve been bruised by life to relax, meet other people of like minds, or to simply sit quietly, knitting or colouring, without fear of being asked to ‘move along.’
Tuesdays and Thursdays, between 2pm and 6pm, Shelley and her husband Jason welcome all to their home loft in Leslieville. Shelley suffers from what her doctor has called complex post traumatic stress disorder caused by childhood trauma. She’s known many people who are unable to cope with modern day life, and who struggle with mental health issues. When a bout of agoraphobia kept Shelley away from being with friends, she realized that she could have her friends come to her, and make everyone happy.
And she certainly has succeeded in her quest. If you are interested in attending, please call 416-821-1754.
Laughter might be the best medicine, but music is a close second, in my case, and I was lucky to get a double dose of the good stuff when our fearless editor and modest rockstar Bob Segarini was persuaded to reunite the Alzeimer Appreciation Orchestra and Chorus for a good cause – we all needed a night out and a hang.
 Musical Director Peter Kashur brought together Bob, Drew Winters, and a motley crew of Kid Carson, Craig Riddock, Connor Walsh, Annette Shaffer and myself for a rollicking 45 minute set that grew, like Topsy, into an hour and a half of bluster and blather.
Musical Director Peter Kashur brought together Bob, Drew Winters, and a motley crew of Kid Carson, Craig Riddock, Connor Walsh, Annette Shaffer and myself for a rollicking 45 minute set that grew, like Topsy, into an hour and a half of bluster and blather.
Despite the terrible weatheriness of the weather, we had a solid crowd of family and friends, and a good time was had by all.
Video courtesy of Jean E. Trivett, aka JeanDaGnu or GnuJet.
Last night was the March 17th Birthday Boy‘s final treat – a Nature Boy salon featuring Jane Siberry, with special guests Mary Margaret O’Hara and Geneviève Marentette.
 The singers, ably accompanied by pianist Michael Shand, performed for an appreciative crowd in a private home in the Annex. These salons are a wonderful way for musicians to make a living, performing in a comfortable setting, where the attendees are fans, grateful for a chance to capture an intimate moment in time with their musical icons, and even have a conversation with them after their show at the reception.
The singers, ably accompanied by pianist Michael Shand, performed for an appreciative crowd in a private home in the Annex. These salons are a wonderful way for musicians to make a living, performing in a comfortable setting, where the attendees are fans, grateful for a chance to capture an intimate moment in time with their musical icons, and even have a conversation with them after their show at the reception.
Ms Siberry did not disappoint, as she wove her musical web over the rapt audience, performing several songs off her new CD, “Angels Bend Closer,” as well as takes on classic tunes such as “Nature Boy” and “The Girl From Ipanema.”
On this evening, Jane was the headliner, but on Friday night, it was Geneviève Marentette’s night to shine, and I’m very sorry to have missed that. I was not familiar with her work, but was impressed with her vocal additions when the three vocalists harmonized. I’m even more impressed since listening to her recent CD “Gigi” and watching her collaborations with luminaries such as David Clayton-Thomas and the much missed Don Francks.
Mary Margaret O’Hara’s Sunday night (tonight) show sold out immediately, and a second show has been added for Monday – but that’s sold out as well. Mary Margaret kept the crowd in stitches throughout the evening, with her trademark yips and sounds. O’Hara’s 1988 release, Miss America, is still regarded as a seminal recording, and the singer has been described as “a force of nature, a remarkable singer and composer whose crystal-clear soprano acrobatics and hypnotic songs defy accepted conventions”
Today the sun is shining, the sky is blue, and it’s supposed to get up to 15 C/59 F today. Time to see if I can still ride the old bicycle without breaking a hip. Yeah, I could get used to this groove, especially living in Toronto, with all that’s offered.
Wave if you see me cycling by!



 I am normally a peaceable, happy person, but lately I’ve discovered just how much rage I have for the blandly evil, those who nonchalantly throw the lives of innocents into turmoil and pain for no more reason than a belief in their own superiority. How angry am I? The next person who shrugs off ANY thing to do with the Orange-Tufted Twitter Flitterer with a casual ‘fake news’ gets it right in the kisser.
I am normally a peaceable, happy person, but lately I’ve discovered just how much rage I have for the blandly evil, those who nonchalantly throw the lives of innocents into turmoil and pain for no more reason than a belief in their own superiority. How angry am I? The next person who shrugs off ANY thing to do with the Orange-Tufted Twitter Flitterer with a casual ‘fake news’ gets it right in the kisser. The #SwoleLeft was started by 26 year old New Yorker, Poncho Martinez, who says: “Trump’s election made it clear that the Democrats are incompetent—that their power machinations are useless when confronted with a different fighting style, and that regular people need to get involved with politics on an individual level and on a daily basis.”
The #SwoleLeft was started by 26 year old New Yorker, Poncho Martinez, who says: “Trump’s election made it clear that the Democrats are incompetent—that their power machinations are useless when confronted with a different fighting style, and that regular people need to get involved with politics on an individual level and on a daily basis.” However, if The Trump of Doom is correct that fake news is the enemy of the people, then he has made himself Public Enemy Number One, through his dedication to the spreading of complete fabrications and outright lies, while offering no evidence to back up his take on what he’s seen on FOX or what he’s heard from some German golfer who knows a guy who knows a guy. We are, in the words of KellyAnne “WrongWay” Conway, to take his tirades and rants, not as mere prose, like ordinary people use, but as some sort of special messages he is delivering from his heart. You know, like that other guy, the North Korean Dear Leader, that is so misunderstood outside of his own country.
However, if The Trump of Doom is correct that fake news is the enemy of the people, then he has made himself Public Enemy Number One, through his dedication to the spreading of complete fabrications and outright lies, while offering no evidence to back up his take on what he’s seen on FOX or what he’s heard from some German golfer who knows a guy who knows a guy. We are, in the words of KellyAnne “WrongWay” Conway, to take his tirades and rants, not as mere prose, like ordinary people use, but as some sort of special messages he is delivering from his heart. You know, like that other guy, the North Korean Dear Leader, that is so misunderstood outside of his own country. There is misinformation, and there is propaganda; there is a ‘sex sells’ slant, and ‘if it bleeds it leads.” And then there is the $2 billion worth of media attention, about twice the all-in price of the most expensive presidential campaigns in history, that was given to Mr. So-Called-President gratis during the last campaign, allowing him to outline his plans to Make America Great Again.
There is misinformation, and there is propaganda; there is a ‘sex sells’ slant, and ‘if it bleeds it leads.” And then there is the $2 billion worth of media attention, about twice the all-in price of the most expensive presidential campaigns in history, that was given to Mr. So-Called-President gratis during the last campaign, allowing him to outline his plans to Make America Great Again. Dire Abbey has his own personal vision of America, which is apparently a place of carnage, a dumpster fire of cataclysmic proportions, where the citizens flee in terror of one another and certainly from anyone of any sort of colour that is not orange. Which is odd, because it would seem that he has seen very little of the country he represents, beyond the golden toilets of his suites in Mar A Lago or New York city, or as seen through the tinted windows of his private jet. Is this ‘dumpster fire’ visible from his unfriendly skies when he can tear his eyes away from Bill O’Reilly?
Dire Abbey has his own personal vision of America, which is apparently a place of carnage, a dumpster fire of cataclysmic proportions, where the citizens flee in terror of one another and certainly from anyone of any sort of colour that is not orange. Which is odd, because it would seem that he has seen very little of the country he represents, beyond the golden toilets of his suites in Mar A Lago or New York city, or as seen through the tinted windows of his private jet. Is this ‘dumpster fire’ visible from his unfriendly skies when he can tear his eyes away from Bill O’Reilly? His dystopic vision was nurtured on the ramblings of alt-right ‘celebrities,’ and misspelled internet memes, which does, in some horrific way, make him representative of half of the American people. And it is the internet that must bear responsibility for the care and nurturing of trolls and hackers who gleefully terrorize social media like the bullies at a Nerd Prom.
His dystopic vision was nurtured on the ramblings of alt-right ‘celebrities,’ and misspelled internet memes, which does, in some horrific way, make him representative of half of the American people. And it is the internet that must bear responsibility for the care and nurturing of trolls and hackers who gleefully terrorize social media like the bullies at a Nerd Prom. You have been warned. Next time … POW!
You have been warned. Next time … POW!
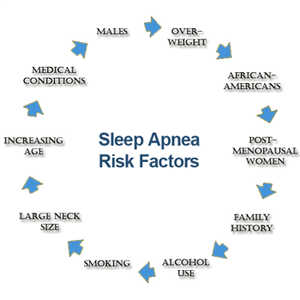 Sleep apnea is a disorder that anyone can experience, even little kids. But it’s more likely to happen if you’re male, over 40, overweight, and have a family history. It’s also common in those who suffer from gastric reflux, or who have a history of allergies, sinus problems, a deviated septum, large tonsils, a large tongue, or a small jaw bone. Having a larger neck (17 inches or greater in men and 16 inches or greater in women) may indicate problems as well.
Sleep apnea is a disorder that anyone can experience, even little kids. But it’s more likely to happen if you’re male, over 40, overweight, and have a family history. It’s also common in those who suffer from gastric reflux, or who have a history of allergies, sinus problems, a deviated septum, large tonsils, a large tongue, or a small jaw bone. Having a larger neck (17 inches or greater in men and 16 inches or greater in women) may indicate problems as well. with my jammies. And so, one cold and snowy night, me and my footie pyjamas were ushered into what looked like a budget motel room, where I filled in numerous forms and was then weighed and measured, before being hooked up to the machine that doesn’t go ‘ping!’
with my jammies. And so, one cold and snowy night, me and my footie pyjamas were ushered into what looked like a budget motel room, where I filled in numerous forms and was then weighed and measured, before being hooked up to the machine that doesn’t go ‘ping!’ or earlobe monitors your heart rate and the level of oxygen in your blood. None of these devices are painful. They are all designed to be as comfortable as possible. The sensors may feel strange on your skin at first. But most people get used to them very quickly. They should not be an obstacle that keeps you from falling asleep. After everything is hooked up, you will do a test to make sure it is all in working order. You will be asked to move your eyes, clench your teeth and move your legs. Once it is all ready, you are free to read or watch TV until your normal bedtime. Then the lights are turned out and it is time for you to go to sleep.”
or earlobe monitors your heart rate and the level of oxygen in your blood. None of these devices are painful. They are all designed to be as comfortable as possible. The sensors may feel strange on your skin at first. But most people get used to them very quickly. They should not be an obstacle that keeps you from falling asleep. After everything is hooked up, you will do a test to make sure it is all in working order. You will be asked to move your eyes, clench your teeth and move your legs. Once it is all ready, you are free to read or watch TV until your normal bedtime. Then the lights are turned out and it is time for you to go to sleep.” ng that you pass or fail. The scored results are simply given to a doctor for further evaluation. At an accredited center, this doctor must be a board-certified sleep specialist. The doctor will review the study to find out what kind of sleep problem you may have. Because of the detail and amount of time involved, it usually takes about two weeks for you to get the results. The doctor who ordered the study will discuss the results with you. If your primary care doctor ordered it, then the results are sent to him or her. If you met with a doctor in the sleep center, then he or she will tell you the results.”
ng that you pass or fail. The scored results are simply given to a doctor for further evaluation. At an accredited center, this doctor must be a board-certified sleep specialist. The doctor will review the study to find out what kind of sleep problem you may have. Because of the detail and amount of time involved, it usually takes about two weeks for you to get the results. The doctor who ordered the study will discuss the results with you. If your primary care doctor ordered it, then the results are sent to him or her. If you met with a doctor in the sleep center, then he or she will tell you the results.” This is a mask that will either cover your nose or your nose and mouth. Another version has soft silicone tubes, called nasal pillows, which fit directly in your nostrils, and provide a steady stream of air that gently blows into the back of your throat. This treatment is called positive airway pressure (PAP). While there are three kinds of PAP, the most common uses a level of pressure that remains continuous (CPAP.) In Canada, Health Insurance subsidizes a percentage of the cost, but, depending on the model you choose to buy, you’re looking at shelling out somewhere between $200 and $1000.
This is a mask that will either cover your nose or your nose and mouth. Another version has soft silicone tubes, called nasal pillows, which fit directly in your nostrils, and provide a steady stream of air that gently blows into the back of your throat. This treatment is called positive airway pressure (PAP). While there are three kinds of PAP, the most common uses a level of pressure that remains continuous (CPAP.) In Canada, Health Insurance subsidizes a percentage of the cost, but, depending on the model you choose to buy, you’re looking at shelling out somewhere between $200 and $1000. est case scenario might mean a vast improvement in your health and overall enjoyment of life.
est case scenario might mean a vast improvement in your health and overall enjoyment of life.










